Beyond experimental tooling, algorithmic diagnostics are maturing into essential healthcare infrastructure, creating a distinct window for strategic allocation.
KEY TAKEAWAYS FOR INDUSTRY LEADERS
- Infrastructure Over Product: AI diagnostics have shifted from optional clinical tools to the foundational architecture of care delivery. Control over this layer now equates to control over patient access and routing.
- Massive Market Expansion: The sector is set to grow from $21.66 billion in 2025 to over $110 billion by 2030, driven not by hype, but by structural necessity.
- Commoditization of Precision: With diagnostic accuracy becoming a baseline expectation (e.g., 94% sensitivity in lung nodules vs. 65% human baseline), competitive advantage has migrated to system integration and workflow orchestration.
- The “Pre-Patient” Economy: New revenue models are emerging in pre-symptomatic risk stratification, allowing organizations to capture value before traditional clinical cycles even begin.
- Urgent Capital Pivot: Executives must shift investment from fragmented pilot programs to interoperability middleware and strategic partnerships that secure ownership of the care coordination infrastructure.
The diagnostic landscape in healthcare is undergoing a fundamental reconfiguration. What began as experimental algorithmic assistance has evolved into the foundational architecture through which care is accessed, triaged, and delivered. This transformation represents more than technological advancement; it signals a permanent displacement of traditional diagnostic economics.
The mandate for executive leadership has shifted from passive observation of innovation trends to active architectural decision-making. Organizations positioning these capabilities as externally managed utilities risk surrendering their most strategic asset: control over the patient care pathway. The evolution of AI diagnostics is no longer defined by isolated technical breakthroughs. It is increasingly characterized by breadth, acceleration, and cross-specialty penetration, all hallmarks of an industry approaching structural scale. Unlike previous hype cycles, current adoption metrics reflect sustained utility rather than speculative interest.
Market Growth & Opportunity
The global AI healthcare market is projected to grow from $21.66 billion in 2025 to over $110 billion by 2030, with diagnostic applications representing a core growth driver. By 2030, algorithmic diagnostic capability will constitute baseline care delivery infrastructure.
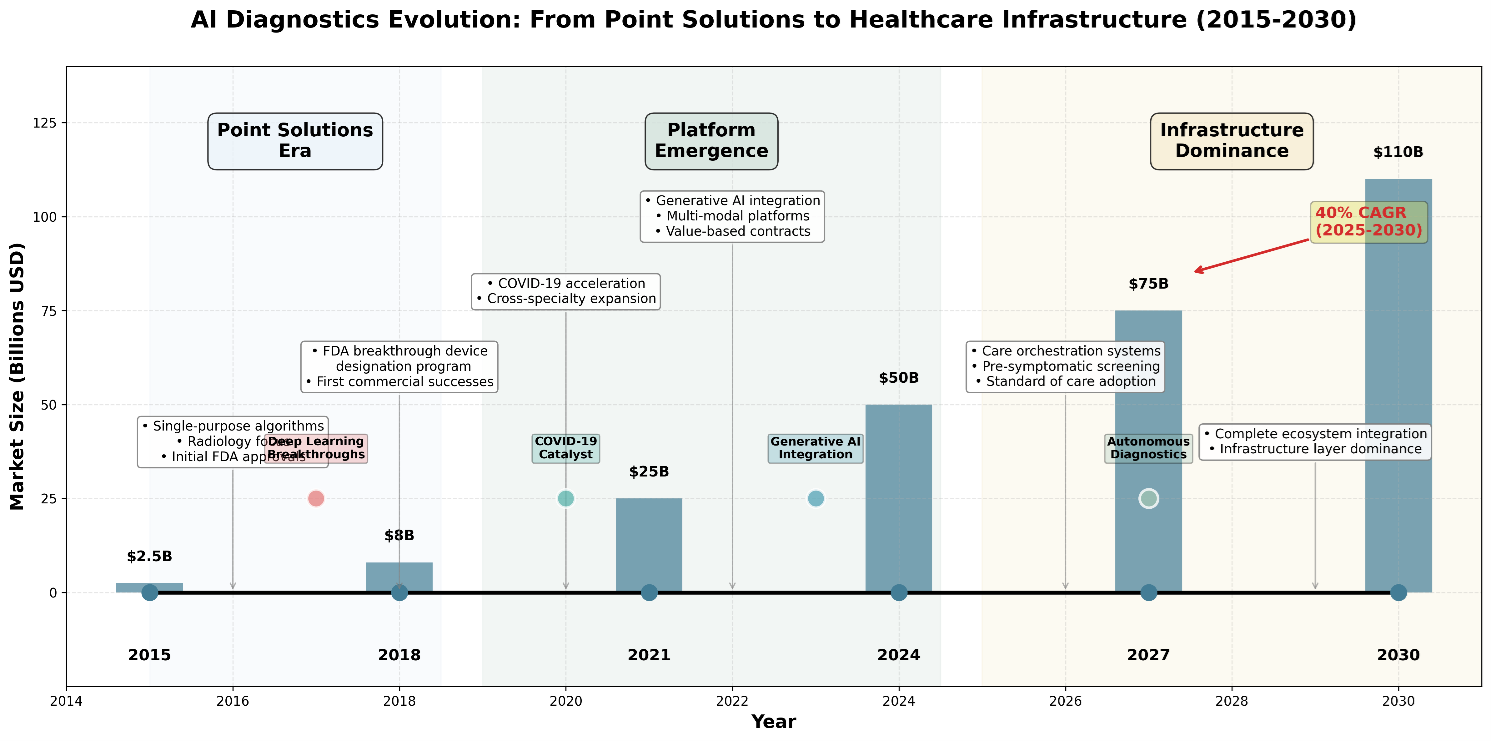
Figure 1: Diagnostic AI Evolution Timeline (2015-2030) – The shift from point solutions to infrastructure dominance.
Early activity concentrated heavily in radiology, which served as the initial proving ground. That concentration is visible in sustained growth from the mid-2010s onward, establishing radiology as the foundation layer for clinical AI adoption. More importantly, this early success unlocked confidence, regulatoryprecedent, and workflow acceptance that would later enable expansion beyond imaging.
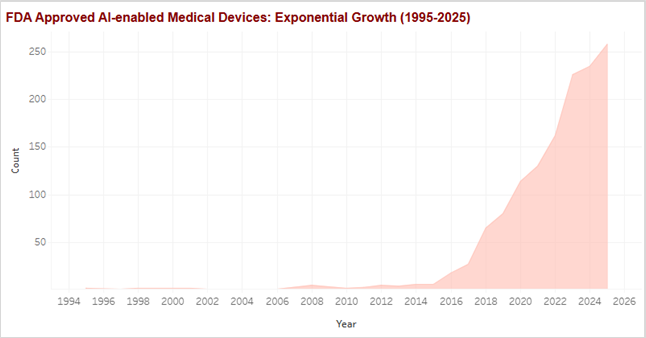
Figure 2: FDA-Approved AI-Enabled Medical Devices Trend – Exponential growth acceleration post-2018.
The Infrastructure Transformation
The prevailing classification of diagnostic algorithms as clinical performance enhancer tools merely accelerating radiologist or pathologist throughput represents a fundamental misunderstanding of the transition underway. The trajectory follows a distinct pattern: discrete products evolving into integrated platforms, ultimately crystallizing as infrastructure.
During the initial deployment phase between 2015 and 2022, these technologies functioned as isolated applications identifying specific pathologies within constrained domains. The current generation represents a qualitative departure. Advanced generative architectures now synthesize disparate data modalities (diagnostic imaging, genetic sequencing, longitudinal health records) into unified stratification frameworks, moving beyond detection toward comprehensive risk interpretation.
The counterintuitive reality is that diagnostic precision has commoditized. With regulatory pathways accelerating and algorithmic performance exceeding human baseline metrics across multiple specialties, superior accuracy alone provides no sustainable advantage. The new competitive axis is systemic integration. Point solutions represent liability; coordinated diagnostic ecosystems that autonomously stratify, route, and sequence patient interventions constitute defensible strategic positioning.
Clinical Applications Driving Adoption
These AI technologies aren’t just theoretical concepts; they are already being integrated into hospitals and labs, fundamentally changing how doctors diagnose diseases in four key areas:
1. Seeing the Invisible in Medical Images
Radiology is one of the fields where AI has made the most significant impact, analyzing X-rays, CT scans, and MRIs with superhuman speed and accuracy.
- Detecting Lung Nodules: In a collaboration between Massachusetts General Hospital and MIT, an AI system achieved a 94% accuracy rate detecting lung nodules on scans, a significant leap over the 65% accuracy achieved by human radiologists in the same task.
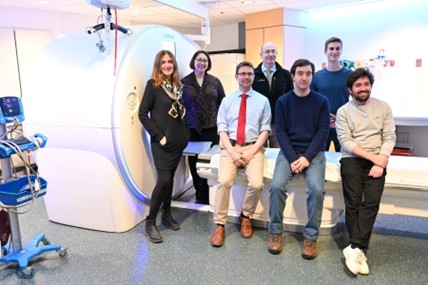
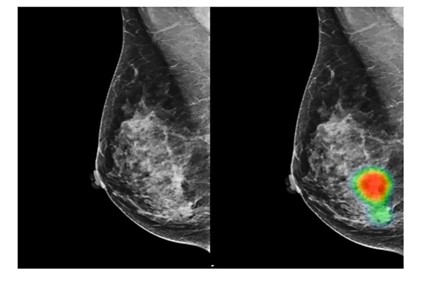
- Finding Breast Cancer: A South Korean study found that an AI-based tool achieved 90% sensitivity in detecting breast cancer with mass, outperforming radiologists who achieved 78%. The same system also demonstrated superior capabilities in early breast cancer detection with 91% accuracy compared to radiologists at 74%.
2. Decoding DNA for Personalized Medicine
Genomics is getting a turbo boost. AI rips through unique genetic data to tailor treatments. Take medulloblastoma, AI analyzed hundreds of profiles to find specific molecular subgroups, allowing doctors to dose precisely for that patient’s specific cancer type. AI cancer detection tools are now matching expert tumor board recommendations 93% of the time.
3. Predicting the Future of Patient Health
AI excels at predictive analytics by analyzing patterns in patient data to forecast what might happen next. Collaborations between institutions like Johns Hopkins Hospital and Microsoft Azure AI trained algorithms on vast amounts of information from EHRs, medical imaging, and genomics to predict patient outcomes like disease progression and readmission risks.
4. Speeding Up Emergency Care
In critical situations like a stroke, every minute counts. AI-powered tools from Aidoc have led to a 34% reduction in door-to-puncture (DTP) time for stroke patients, equivalent to 38 minutes saved. This accelerated process allows clinicians to act faster, reducing brain damage and significantly improving recovery chances
Tangible Benefits & ROI
The powerful applications of AI lead to three major benefits that are reshaping the patient experience and the efficiency of the entire healthcare system.
| Benefit | What It Means for Patients | The Proof & Business Impact |
| Greater Accuracy | Fewer mistakes, catching disease earlier when it’s fixable. | ~32% of US adult population lost life due to medical error such as fatal drug doses. AI cuts this down by eliminating fatigue and bias. [Johns Hopkins Medicine] |
| Faster Efficiency | Less waiting, faster treatment. Crucial in emergencies. | One diagnostic chain used the Scispot platform to cut workflow errors by 40% and gave patients instant reports. [Scispot Platform] |
| Optimized Costs | Automating grunt work cuts costs and expands access. | The industry could save $200 billion to $360 billion annually. That is real capital released for better care. [McKinsey & Company] |
Structural Market Drivers
Growth in AI diagnostics is underpinned by non-cyclical, systemic forces that insulate the sector from broader macroeconomic volatility.
- Workforce Crisis: With global health workforce gaps projected to reach 10 million practitioners by the decade’s end, according to the World Health Organization, the economics of human-dependent diagnostic scaling have become structurally unviable. Algorithmic augmentation is no longer a luxury but an operational necessity.
- Episode-Based Economics Collapse: Traditional fee-for-service structures cannot absorb the labor economics required for continuous patient monitoring. Value-based reimbursement mandates high-frequency surveillance economically feasible exclusively through algorithmic automation. Diagnostic intelligence has effectively eliminated marginal cost at scale.
- Data Utility Inversion: Historical value concentration around patient record custody is migrating toward platforms capable of executing actionable interventions. Generative capabilities that synthesize unstructured clinical data render passive information repositories less valuable compared to active diagnostic processing layers.
The Competitive Landscape & Whitespace
With diagnostic precision commoditized, capital allocation priority shifts toward domains where competitive differentiation remains achievable. The market presents substantial opportunity in care coordination governance and execution infrastructure.
Clinical Deferral Logic: The Orchestration Intelligence Layer
The highest-value intellectual property will not reside in diagnostic algorithms themselves, but in the decision frameworks governing their deployment. The strategic opportunity lies in developing proprietary routing intelligence that channels routine cases to algorithmic processing while directing complex presentations to specialized clinical review. This routing infrastructure functions as operational traffic control, the coordination mechanism determining institutional throughput and resource utilization.
Pre-Symptomatic Risk Stratification: Capturing the “Pre-Patient”
Conventional diagnostic frameworks operate reactively, engaging after symptom manifestation. The emerging value frontier involves synthesizing genetic predisposition data with longitudinal imaging patterns to project disease probability trajectories before clinical presentation. This approach relocates health system engagement earlier in the patient journey, effectively expanding the addressable market into pre-disease populations.
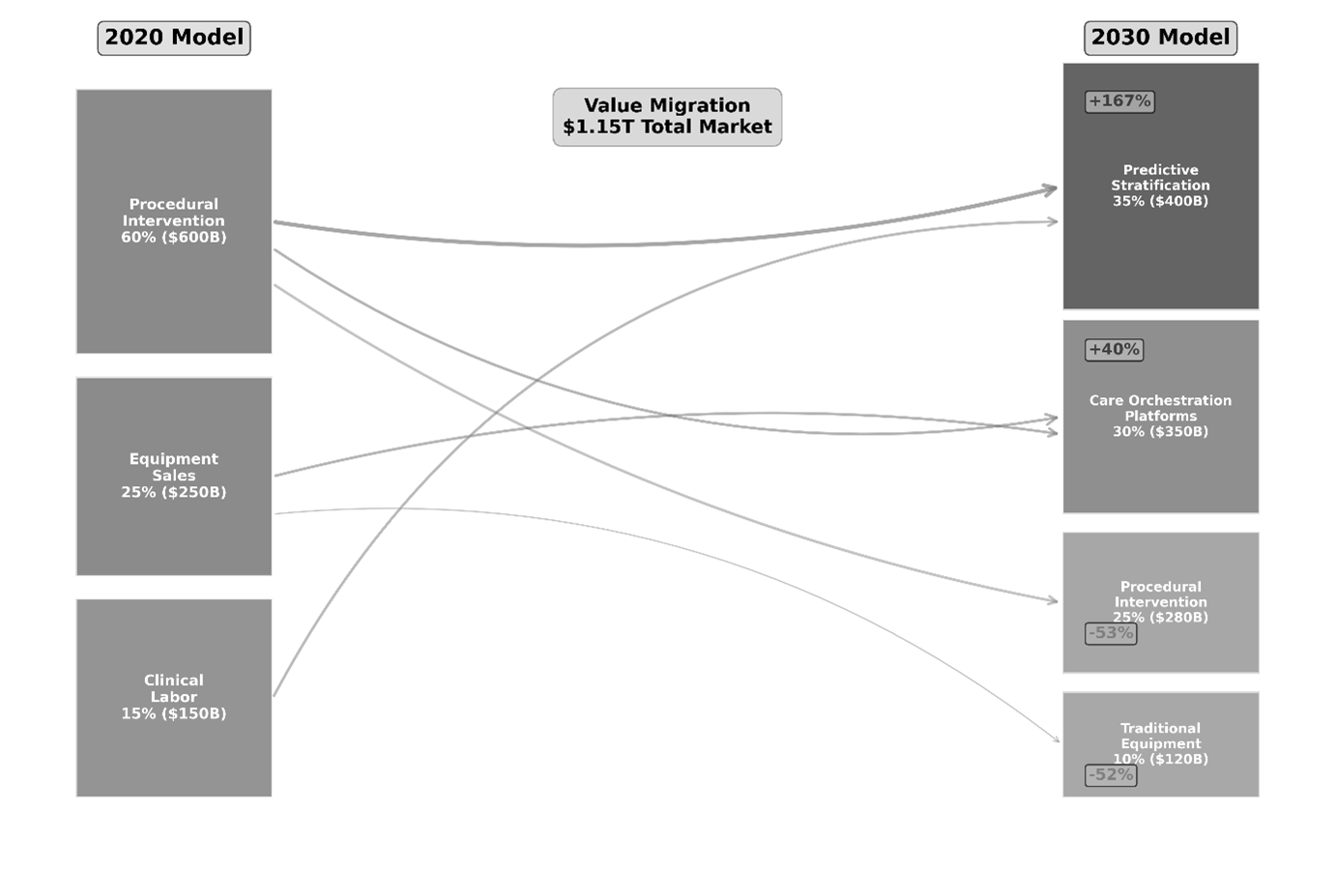
Figure 3: Healthcare Value Migration (2020-2030) – Margin capture shifting toward predictive stratification.
The Human-AI Partnership Model
The most effective approach for AI in medicine is collaboration, not replacement. Research from Google DeepMind on a system called CoDoC (Complementarity-driven Deferral-to-Clinical Workflow) proves the power of this partnership.
The system is designed to learn when to rely on the AI’s prediction and when to “defer to a clinician.” In one test scenario using a large mammography dataset, this collaborative approach reduced the number of false positives by 25% compared to standard clinical workflows, all without missing any true positive cases. This ensures that the final decision is always made using the best of both worlds.

